Blog
Uterine cancer markers: what they can show and what you shouldn't expect from them
When people search for information about uterine cancer markers, they often expect that there is one accurate blood test that will either confirm or rule out the disease. But in practice, things are not so simple. First, the phrase «uterine cancer» is often used to refer to different conditions: cancer of the uterine body, that is, endometrium, and cervical cancer. Second, the approaches to their detection differ. There is no standard routine screening test for endometrial cancer, and for cervical cancer, the main tools remain the HPV test and the PAP test, not the blood test for tumor markers.
The most important thing to know right away: Blood tumor markers generally don't work very well as a screening tool for people without symptoms. The National Cancer Institute states bluntly that circulating tumor markers are often not sensitive or specific enough to detect early, asymptomatic cancers. That's why a normal or elevated level alone doesn't make or break a diagnosis.
Is there a single marker for uterine cancer?
No, there is no single universal marker for uterine cancer. In the case of endometrial cancer, in some clinical situations, they may be used CA-125, but it is not a screening test or a test that confirms cancer on its own. The Mayo Clinic notes that CA-125 can be used to monitor endometrial cancer, but it can also be elevated in noncancerous conditions, including endometriosis, liver disease, menstruation, pelvic inflammatory disease, pregnancy, and uterine fibroids.
When it comes to cervical cancer, the role of «markers» in the usual sense is not played by proteins in the blood, but by the results of HPV test і Pap test. The CDC explains that the HPV test looks for the human papillomavirus, which can cause changes in cervical cells, while the Pap test looks for precancerous or abnormal cells. A positive HPV test does not mean cancer is present, and an abnormal Pap test usually does not automatically mean cancer.
Table: which «markers» and tests are actually used
| Situation | What matters most often | What is important to understand |
|---|---|---|
| Suspected endometrial cancer | Symptom assessment, imaging, endometrial sampling/biopsy, sometimes CA-125 | CA-125 is not a screening test «just in case» |
| Endometrial cancer already confirmed | CA-125 can help assess the course or response to treatment | Elevated CA-125 does not always mean cancer, and a normal level does not rule it out. |
| Suspected cervical cancer or preventive screening | HPV test and PAP test | These are the main tools for early detection of cervical changes. |
| Suspected cervical cancer after abnormal tests | Colposcopy and biopsy | The final answer comes from tissue, not a blood test |
This logic follows from the clinical recommendations of the NCI, CDC, Mayo Clinic, and American Cancer Society: there is no routine screening for endometrial cancer, HPV/PAP are key for the cervix, and the diagnosis of suspected cancer is confirmed on tissue.
If it is cancer of the uterine corpus
Endometrial cancer is often detected not by a tumor marker but by symptoms. The NCI and Mayo Clinic indicate that the most common signs are abnormal vaginal bleeding, spotting between periods, or bleeding after menopause; this is why many cases are found relatively early. There is no routine, standard screening test for endometrial cancer.
When a doctor truly suspects endometrial cancer, it is not a «blood marker» but a tissue test that is decisive. The NCI describes endometrial sampling as the removal of tissue from the endometrium for examination under a microscope, and the American Cancer Society notes that endometrial biopsy is one of the most widely used and highly accurate tests for diagnosing endometrial cancer. That is, with real suspicion, the main step is morphological confirmation, not the search for a universal tumor marker.
If it is cervical cancer
The situation is different for the cervix. Here the most important things are: HPV test і Pap test, because they help find precancerous changes or detect cancer risk early. The CDC specifically states that these two tests can help prevent cervical cancer or find it early. The HPV test looks for the virus, while the Pap test looks for changes in cervical cells.
If the results are alarming, the next step is not «another marker in the blood,» but a follow-up examination of the cervix. The NCI notes that colposcopy often includes a biopsy, and a biopsy is the procedure in which a pathologist checks the tissue for signs of cancer. It is this that provides the final answer when a malignant process is suspected.
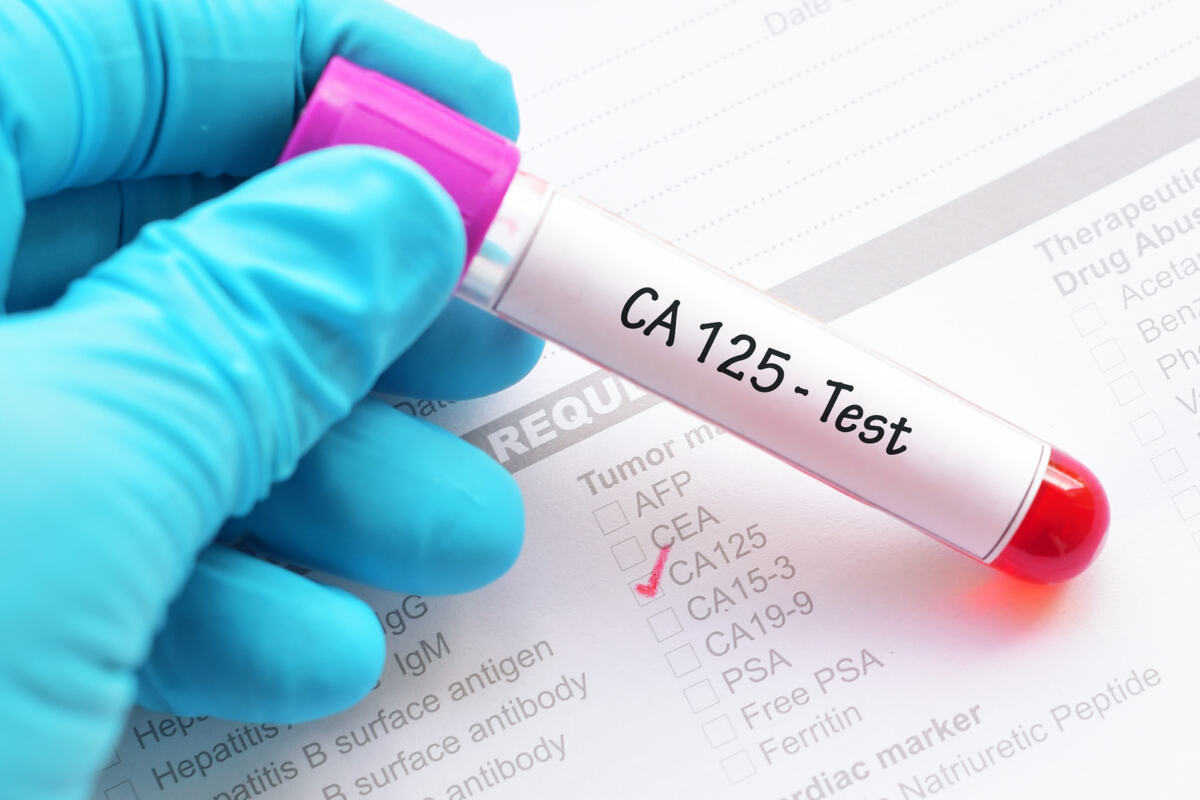
When CA-125 can still be useful
CA-125 sometimes referred to in the context of "uterine cancer markers," and that's not entirely wrong, but accuracy is important. The Mayo Clinic states that this test can be used to endometrial cancer to monitor the course of the disease or treatment. The NCCN patient materials also state that high CA-125 may indicate that the tumor has spread beyond the uterus. But this does not make CA-125 a good universal test for early detection in everyone.
That is, CA-125 is more of an auxiliary marker in an already suspected or confirmed situation than a test for preventive «check-ups.» That is why taking this test on your own without symptoms and without a clinical inquiry often does not provide the clarity that people expect.
What is important to remember
Simply put, uterine cancer markers — it’s not just one button in the laboratory. For the uterine body, symptoms, ultrasound, and endometrial biopsy; CA-125 can be an auxiliary, but not the main screening test. For the cervix, the HPV test and the PAP test are key, and if cancer is suspected, a biopsy gives the final answer.
Therefore, the most useful approach is not to look for «one definitive marker,» but to understand what type of uterine cancer you have and what testing really makes sense in your situation. This tactic is usually more useful than a random blood test without a clear clinical question.


