Blog
Early cancer diagnosis: what really works
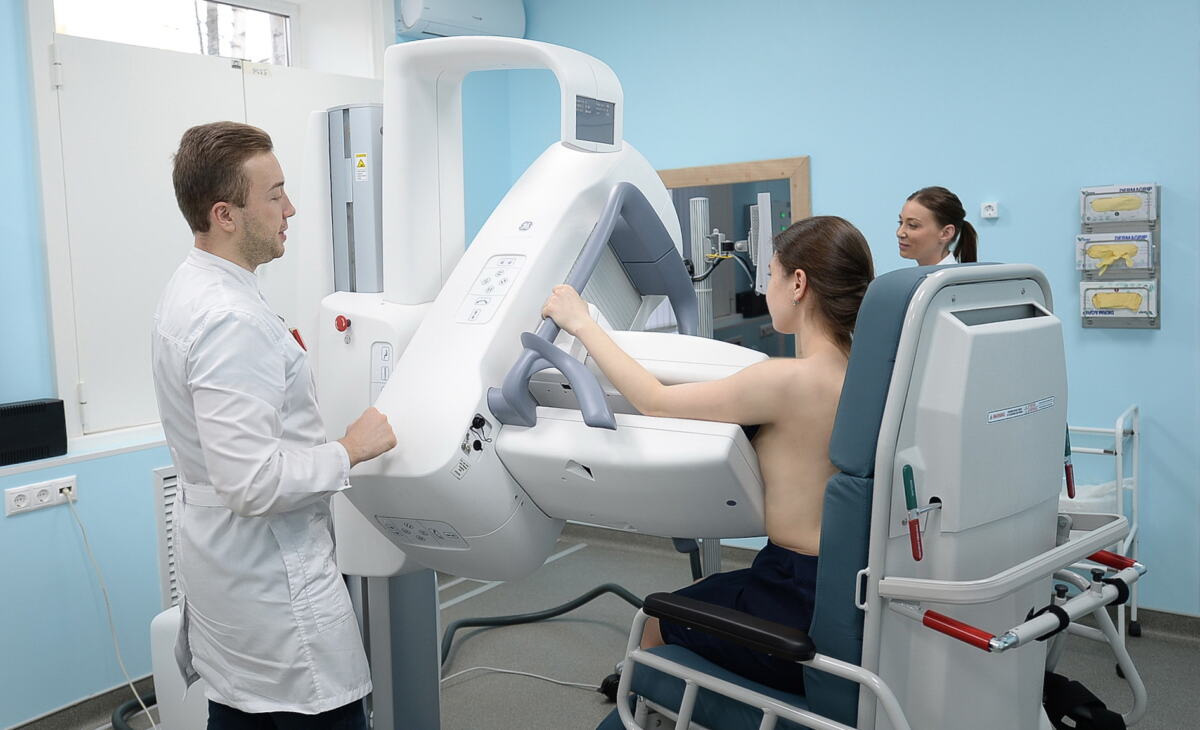
Early diagnosis of cancer — is not one “universal test”, but a whole system of actions that helps to find the disease as early as possible. It consists of two different directions: early detection of cancer in people who have already developed symptoms, and screening in people without symptoms, if there is a proven examination method for a certain type of cancer. This approach is considered the basis of modern cancer prevention, because early detection increases the chances of more effective treatment, less complexity of therapy and a better prognosis.
The most common mistake is to look for a “one-size-fits-all test” or to think that early cancer diagnosis is equal to a package of tumor markers. In fact, evidence-based medicine works differently: for some tumors there are screening methods that have proven beneficial, and for others the main thing is not to miss alarming symptoms and consult a doctor in time. The US National Cancer Institute directly notes that only some screening tests have a proven ability to detect cancer early and reduce the risk of death from it.
What is included in early cancer diagnosis?
Below is a short table that explains the logic of early diagnosis well. It summarizes the approaches used in international guidelines for the most common oncological diseases.
| Direction | For whom | What can be included |
|---|---|---|
| Breast cancer screening | People without symptoms in certain age groups | Mammography |
| Colorectal cancer screening | People without symptoms at the recommended age | Fecal occult blood tests, FIT, colonoscopy, or other approved methods |
| Cervical cancer screening | People without symptoms with cervical cancer | Pap test, HPV test, or cotest depending on age and guidelines |
| Lung cancer screening | Only high-risk groups | Low-dose CT scan if there is a significant smoking history |
| Early detection of symptomatic cancer | People who already have complaints | Doctor's examination, imaging, endoscopy, biopsy and other targeted examinations |
What methods have proven benefits?
For breast cancer, mammography remains one of the most important early detection methods. The current USPSTF recommendation recommends that women ages 40 to 74 have screening mammography every two years. This is one of the best-studied screening approaches in oncology.
For colorectal cancer, screening is recommended to begin at age 45 and continue until age 75, and the format of the examination can vary: from stool tests to colonoscopy. What is important here is not which method is “more fashionable,” but that the person is generally covered by screening and does it regularly.
For cervical cancer, the Pap test, HPV test, or both are used, depending on age and specific guidelines. Both the CDC and NCI emphasize that these tests help either prevent cervical cancer or find it early. It is important to follow the recommended schedule and not get tested haphazardly.
Early detection is also available for lung cancer, but it is not suitable for everyone. Annual low-dose CT is recommended for people aged 50–80 years with at least a 20 pack-year smoking history who are current smokers or have quit less than 15 years ago. It is not used as a routine screening for people without this risk.
What symptoms should not be ignored?
Early detection of cancer is not only about preventive examinations, but also about paying attention to your body's signals. Symptoms that should not be delayed include a new lump or swelling, blood in the stool or urine, unexplained weight loss, severe or prolonged fatigue, a persistent cough, changes in bowel habits, unusual bleeding, difficulty swallowing, a wound that does not heal, or persistent skin changes. This does not mean that any of these symptoms are necessarily related to cancer, but such changes are considered a reason not to postpone the consultation.
It is also important to remember that some cancers may not have any symptoms at all in their early stages. For example, cervical cancer often has no obvious symptoms in its early stages, so regular screening is especially important here. That is why early cancer diagnosis always relies on two things at the same time: proper screening where it has been proven to be beneficial, and prompt response to unusual symptoms.
What is often mistakenly considered early diagnosis
Early cancer diagnosis does not include random testing tumor markers “for prevention” if there are no clear indications for this. Also, evidence-based screening methods should not be replaced with random “checkups” that are not tied to age, gender, risk factors, or symptoms. Early diagnosis works when it is targeted: the right method — to the right person — at the right time.
The best strategy for a patient is not to look for the worst-case scenarios, but to have a clear plan: know your risk factors, do not skip the recommended screening, and do not ignore changes in well-being that do not go away. This is how early cancer diagnosis stops being an abstract phrase and becomes a real opportunity to detect the problem at a time when the chances of successful treatment are greater.


