Medilab+
Laboratory diagnostics of asthma: accuracy that helps you breathe freely
Asthma: not one disease, but several variants of the course Bronchial asthma is not only shortness of breath and an inhaler. It is a chronic inflammation of the respiratory tract, which can be allergic, non-allergic, mixed, eosinophilic, infection-dependent, aspirin-dependent. Laboratory studies are the key to understanding which type the patient has and which treatment will be effective. Why are laboratory tests prescribed for asthma? To confirm the allergic nature of the symptoms. To identify the level of inflammation - systemic and local. To conduct differential diagnostics with COPD, pneumonia, parasitosis. To determine whether the patient will respond to inhaled steroids. To monitor the effectiveness of therapy (including biological). To explain frequent exacerbations or "nighttime" symptoms. Tests that form the basis of diagnosis. Complete blood count (CBC). An increase in eosinophils above 300 cells/μl indicates eosinophilic inflammation, characteristic of atopic or severe late-stage asthma. Leukocytosis and accelerated ESR are markers of inflammatory exacerbation, in particular infectious. IgE: total and specific. Total IgE: its increase indicates allergic sensitization. The higher the level -...
Gene mutation test: when, why and what gives the result
Genetic analysis: a tool for prevention and precise treatment Knowing your genes is not a fashion statement, but a real step towards a sensible attitude to health. Modern genetics makes it possible to identify risks even before the first symptoms appear. And a gene mutation test helps with this - an analysis that can change your life strategy, treatment or prevention. As the Mayo Clinic explains, "genetic testing is not a sentence, but it provides knowledge that helps you make informed decisions." This is especially important for people with a family history of oncology, thrombosis or congenital diseases. What the gene mutation test examines The test detects abnormalities in the structure of genes that can cause: hereditary forms of cancer (BRCA1, BRCA2, APC, TP53) blood clotting disorders (F5 Leiden, F2) predisposition to cardiovascular, endocrine, mental disorders carriership of genetic diseases that can be passed on to children The material for analysis is blood, saliva or buccal swab. The results are interpreted by a medical geneticist. When...
Ascorbic acid deficiency: how to recognize the problem at an early stage
Why is vitamin C so important? Ascorbic acid (vitamin C) is not just another trace element in the list of nutrients. It is involved in numerous biochemical reactions: collagen synthesis, regulation of the immune response, iron absorption, protection of cells from free radicals. Without it, the skin loses elasticity, gums bleed, and the immune system fails. Who is at risk of vitamin C deficiency Patients with chronic gastrointestinal diseases People who follow strict diets or exclude fruits/vegetables Smokers (they have lower vitamin C levels due to oxidative stress) Children and adolescents during active growth Elderly people with impaired appetite Unexpected symptoms that may indicate a deficiency Long-term healing of even small scratches Bruises for no reason Fatigue that does not go away after rest Frequent colds Dry and flaky skin Irritability, memory impairment In severe cases, scurvy may develop - a disease accompanied by tissue destruction, tooth loss, hemorrhages, general...
Tumor markers in liver cancer: diagnosis, significance and limits of effectiveness
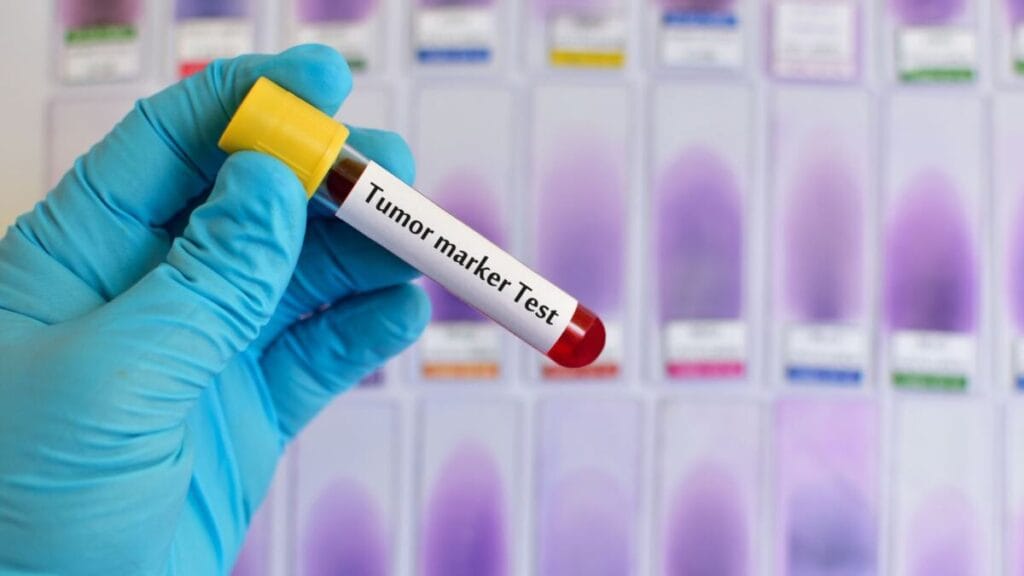
The role of tumor markers in the detection of hepatocellular carcinoma Tumor markers are biological molecules produced by tumor cells or the body in response to the growth of a tumor. In the case of liver cancer, in particular hepatocellular carcinoma (HCC), tumor markers allow you to detect the disease at an early stage, assess the risks of metastasis, and monitor the effectiveness of treatment or possible relapse. Despite the limitations of accuracy, they remain an important component of laboratory diagnostics. The most common tumor markers in liver cancer Alpha-fetoprotein (AFP) This is the main and most frequently used tumor marker in HCC. AFP is produced in the fetal liver, but after birth its level decreases. In adults, elevated AFP levels indicate malignant processes, especially at levels above 400 ng/ml. However, its specificity is limited: not all forms of liver cancer are accompanied by high levels of AFP, and false-positive results are possible in chronic hepatitis or cirrhosis. AFP-L3 (alpha-fetoprotein fraction) This glycoprotein fraction is more specific for hepatocellular carcinoma, as it is mainly synthesized by tumor cells. An increase in AFP-L3 levels even...
Rapid STI tests: a modern approach to self-diagnosis
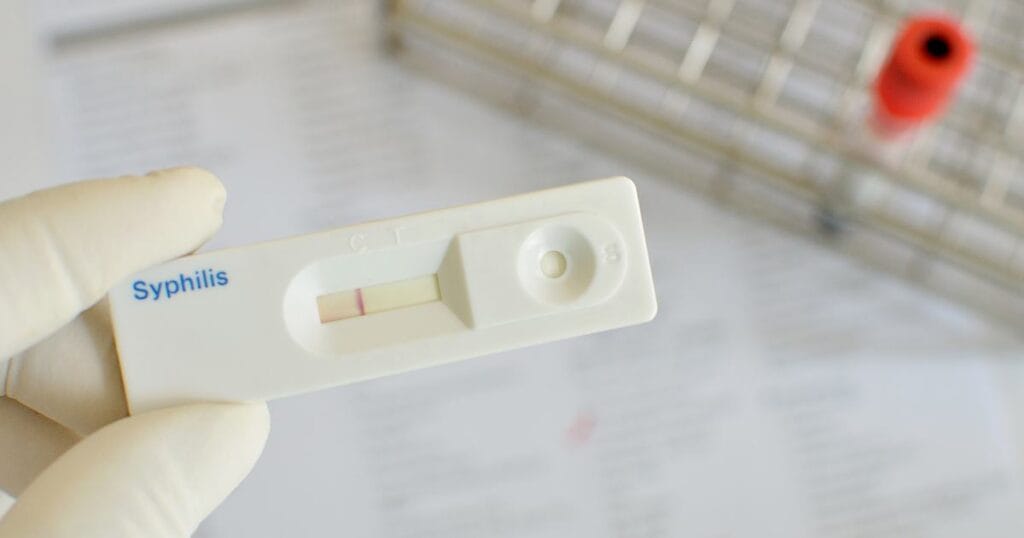
STIs as a health threat Sexually transmitted infections (STIs) remain one of the most global public health problems. According to WHO, more than 1 billion cases of STIs are recorded worldwide each year. The most common of them are chlamydia, gonorrhea, syphilis, human papillomavirus (HPV) and immunodeficiency virus (HIV). Many of these infections may not show symptoms for a long time, making diagnosis difficult. This became the prerequisite for the widespread introduction of rapid tests - a convenient method for detecting STIs at an early stage. What are rapid tests and how do they work Rapid STI tests are diagnostic systems that allow you to detect signs of infections directly in 15–30 minutes. Most often, they detect antibodies (immune response to the pathogen) or antigens (particles of the pathogen itself). A drop of blood, saliva, urine or a swab from the mucous membrane is usually used to conduct the test. The method is similar to rapid tests for COVID-19 or pregnancy: the result is read visually using a colored strip or...
The brain-gut connection: how digestion affects our mood
Have you ever felt "butterflies in your stomach" before an important event? This is not just a figurative expression. Modern science confirms that the brain and gut are closely connected by a complex network of neural, immune and hormonal signals. That is why stress or anxiety can cause digestive disorders, and the state of the intestinal microflora can affect mental health. This phenomenon is called the gut-brain axis. Recent studies show that our mood, behavior and even the risk of developing depression may depend on the state of the intestinal environment. What is the gut-brain axis The gut-brain axis is a two-way communication channel between the central nervous system (brain) and the gastrointestinal tract. Main mechanisms of interaction: Vagus nerve: the main conductor of signals between the brain and the gut Microbiome: billions of bacteria in the gut secrete substances that affect the brain Immune system: changes in the gut can activate an immune response that affects brain function Hormones and neurotransmitters: serotonin, dopamine, GABA - many...
The effect of alcohol on tests
Why alcohol changes test results Alcohol, even in moderate doses, can significantly affect the results of laboratory tests. Its consumption before taking tests can lead to false readings, which complicates diagnosis and treatment. Ethanol affects liver and kidney function, hormonal balance, glucose and lipid levels in the blood. Tests sensitive to alcohol Biochemical indicators and alcohol Alcohol activates the liver, which leads to an increase in enzymes - alanine aminotransferase (ALT), aspartate aminotransferase (AST), gamma-glutamyltransferase (GGT). In practice, a case was recorded when a patient drank wine the day before the test, and his GGT was 98 units/l with a norm of up to 51. A repeated test after 72 hours (without alcohol) showed 47 units/l. Conclusion: alcohol can create a false impression of liver pathologies. Effect on glucose levels Ethanol slows down gluconeogenesis, the process of glucose production by the liver. In a patient with suspected diabetes, after drinking beer before the test, the glucose level dropped to 3.4...
Proteomics: from protein profiles to clinical solutions
Proteomics is the science that studies the proteome, that is, the set of all proteins synthesized by a cell, organ, or organism at a specific point in time. It is a dynamic information system that changes under the influence of environmental conditions, diseases, medications, or stress. It is these changes that provide the key to understanding the mechanisms of diseases, their early diagnosis, and the choice of therapy. From genes to proteins: why the proteome is more important in the clinic While the genome is a permanent structure that reflects hereditary information, the proteome reflects the real activity of the cell. It determines which proteins are formed, in what quantities, what their activity is, and how they interact. Professor Lyudmila Andrusenko, a specialist in molecular biology, notes: «The genome says what can be. The proteome shows what actually is.» Proteomics in medicine: four key directions 1. Biomarkers for early diagnosis Proteins that change their concentration in the early stages of the disease are used as markers. For example, elevated troponin levels are one of...
Anemia test: how to detect iron, vitamin and oxygen deficiency
Anemia is one of the most common conditions in the world. It affects about 30% of the world's population, but often goes unnoticed. A person simply gets used to fatigue, pallor, shortness of breath. And only when the symptoms begin to interfere with work or active living, the question arises: "Isn't this anemia?" In fact, checking is simple. One analysis can give an answer and prevent complications. Anemia: what is it and why diagnostics are important Anemia is a decrease in the amount of hemoglobin or red blood cells in the blood, which leads to impaired oxygen transport. In this case, the body's cells literally "suffocate". The brain, heart, muscles - everything works in oxygen deficiency mode. The consequences are reduced performance, deterioration of cognitive functions, metabolic disorders, organ damage. Early diagnosis of anemia allows not only to restore health, but also to avoid complications such as heart failure, chronic hypoxia of the brain, and decreased immunity. Symptoms of anemia: how they differ in adults, children and pregnant women Anemia manifests itself differently, depending on...
Rare genetic diseases: invisible challenges for medicine and the family
What are rare genetic diseases? Rare (orphan) genetic diseases are diseases that occur in less than 1 in 2,000 people. Most of them are hereditary and manifest themselves in childhood, although some may remain unnoticed until adulthood. Despite the low prevalence of each individual pathology, the total number of patients with rare diseases in the world is millions. In more than 80% of such cases, genetic mutations are the cause. How do these diseases arise? Genetic changes can be: inherited from parents - when both carry a mutant gene (for example, in autosomal recessive inheritance) de novo mutations - arising spontaneously in the embryo as a result of chromosomal rearrangements or point mutations Even a single mutation can change protein synthesis, leading to impaired function of cells, tissues and entire systems. Examples of rare genetic diseases Name of the disease Main manifestations Cystic fibrosis Respiratory distress, frequent infections, digestive problems Rett syndrome Loss of speech and motor skills in girls after 6 months....